If you have a tooth that is seriously infected or damaged, your dentist may have presented you with two options: a root canal or a tooth extraction. Not only can both of these procedures seem intimidating, but it can also be confusing to understand which one is the right choice for you.
While you will ultimately want to consult with your dentist to determine the best option, educating yourself as much as possible allows you to make the most informed decision.
Keep reading to learn more about root canals and tooth extractions and which option may work best for you.
What Is a Root Canal?
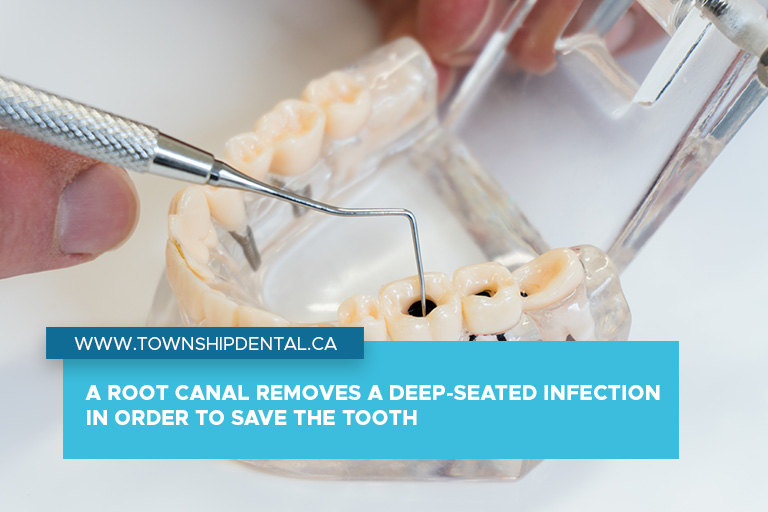
The goal of a root canal is to treat and save a tooth with a damaged or infected pulp, which is the soft tissue at the center of the tooth. The pulp contains nerves, blood vessels, and connective tissue. When it becomes inflamed or infected due to deep decay, a cracked tooth, or repeated dental procedures, it can cause severe pain and lead to the formation of an abscess if left untreated.
Root canals involve removing the infected or damaged pulp from the tooth, cleaning and disinfecting the interior, and filling and sealing the space. The term “root canal” also refers to the natural cavity within the center of the tooth, which houses the pulp. The procedure is typically performed by a dentist or endodontist, a specialist in treating issues related to the tooth’s pulp and surrounding tissues.
When Is a Root Canal the Best Option?
A root canal is often the best choice when a tooth has a deep infection or extensive damage to its pulp, the inner part of the tooth containing nerves and blood vessels. Many people fear root canals due to misinformation about pain and discomfort, but modern techniques and anesthesia have made the procedure relatively painless. Saving a tooth through a root canal is often more cost-effective and less invasive than dental extraction, followed by dental implants or bridges.
In some cases, a root canal can also prevent further complications such as abscesses, bone loss, and the spread of infection to surrounding teeth. Plus, preserving natural teeth through root canals helps maintain proper chewing function and preserves the natural appearance of the smile—things that contribute significantly to overall oral health and well-being.
What Is a Tooth Extraction?

During a tooth extraction, the tooth is removed from its socket in the jawbone. Before the extraction, the dentist will assess the condition of your tooth, often in conjunction with X-rays, to evaluate the roots and surrounding structures.
Once the treatment plan is established, the dentist administers a local anesthetic to numb the area around the tooth. General anesthesia or sedation may be used in more complex cases or for multiple extractions.
With the area properly numbed, the dentist uses specialized instruments, like elevators, to gently loosen the tooth within its socket. The tooth may be carefully rocked back and forth to widen the socket and facilitate its removal. The dentist then grasps the tooth and extracts it from the socket using dental forceps.
After the tooth removal, the dentist may provide post-operative care instructions, including guidelines for managing any discomfort and promoting proper healing. Sometimes, the extraction site may require stitches, and the dentist may recommend follow-up appointments to monitor the healing process.
When Is a Tooth Extraction the Best Option?
A tooth extraction is an ideal option when preserving the natural tooth is no longer feasible or could compromise oral health. Severe tooth decay, extending deep into the pulp chamber and compromising the tooth’s structural integrity, often necessitates extraction when the damage is beyond repair.
Advanced gum disease, causing significant damage to the supporting tissues and bone, may lead to tooth extraction to prevent the spread of infection to adjacent teeth. Irreparable trauma resulting from accidents or fractures may also prompt extraction, especially if the damage extends below the gumline.
Additionally, impacted wisdom teeth, which do not fully erupt or grow in the correct position, often require extraction to prevent potential complications such as pain, infection, or damage to adjacent teeth. In these circumstances, tooth extraction is a necessary and beneficial intervention to maintain oral health and prevent further complications.
Which Option Is Best for You?
As mentioned earlier, you’ll want to consult with a dentist to determine whether you need a root canal or a tooth extraction. In general, however, the extent of damage or infection plays a crucial role.
If the tooth’s pulp is infected, but the overall structure is intact, a root canal might be a viable choice, allowing preservation of the natural tooth. The location of the affected tooth also matters; front teeth are often prioritized for preservation. Your overall oral health and commitment to post-treatment care is also something to consider.
A root canal may be preferred if the surrounding structures are healthy and you can maintain good oral hygiene. But, if the damage is extensive or there’s a risk of infection spreading to nearby teeth and gums, extraction might be recommended.
Need a Tooth Extraction or Root Canal, Get in Touch With Us
Whether you need a tooth extraction or a root canal, the most important thing is that you seek treatment immediately. Neglecting damaged and/or infected teeth doesn’t only impact your oral health; it could have consequences for other areas of your body as well.
At Township Dental, we offer a variety of services, including extractions and root canals in Langley. Request an appointment today, call us at (604) 533-8475.
